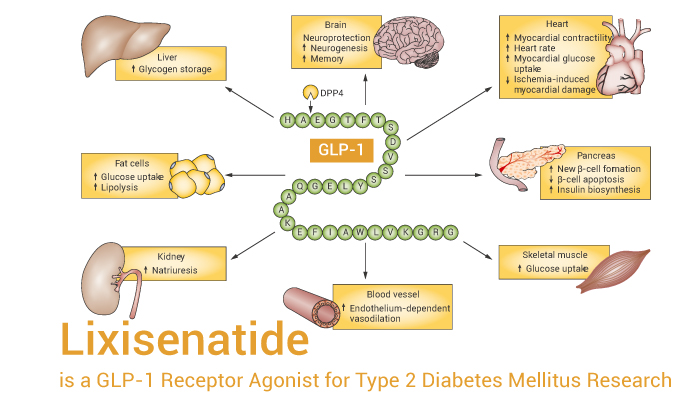
GLP-1 receptor agonists are a class of antidiabetic drugs originally developed for type 2 diabetes. It activates GLP-1 receptors to reduce blood sugar and energy intake, mimicking the effects of GLP-1 released from the intestines after eating. These include: inhibiting glucagon secretion, promoting insulin release, and slowing gastric emptying and increasing satiety. However, some cardiovascular safety profiles have not yet been successfully demonstrated. Here we introduce a potent GLP-1 analogue, Lixisenatide. It is effective in reducing glycated hemoglobin levels in patients with type 2 diabetes by reducing fasting and postprandial blood sugar levels.
Lixisenatide serves as a GLP-1 agonist, can effectively increase insulin secretion and lower blood sugar.
Lixisenatide (3-10 μg/kg; ip; single dose) increases insulin secretion, promotes gastric emptying, activates vagal nerve activity, and brain c-Fos activity in diabetic mice fed different types of high-fat diets. Resulting in a decrease in blood glucose in a naive, chronically vagotomized, GLP-1 receptor knockout (KO) mouse model.
Lixisenatide also has anti-inflammatory, neuroprotective, and renoprotective activities. Downregulate pro-inflammatory cytokines and block cell signaling pathways to inhibit inflammatory responses. For example, (10-20 μM, 48 h) inhibits the activation of IL-1β pro-inflammatory pathways and the expression of IL-1β-induced MMPs in fibroblast-like synoviocytes. Lixisenatide (100 μM, 24 h) alleviates the Aβ25-35-activated Akt–MEK1/2 pathway in hippocampal cells and also inhibits Aβ25-35-induced cytotoxicity. Lixisenatide (1 nmol/kg/day, ip, 14 days) is renoprotective in experimental early diabetic nephropathy in an in vivo model. In mice, it (10 μg/kg/day, sc, 1 month) reduces atherosclerotic burden and systemic inflammation.
In summary, Lixisenatide is a versatile GLP-1 agonist with glycemic, anti-inflammatory activity, and neuroprotective effects.
References:
[1] Pfeffer MA, et al. N Engl J Med. 2015 Dec 3;373(23):2247-57.
[2]. Cai H Y, et al. Behavioural brain research, 2017, 318: 28-35.
[3]. Vinué Á, et al. Diabetologia, 2017, 60: 1801-1812.