Renal ischemia/reperfusion injury (IR) is a major clinical problem found in shock, renal transplantation and other clinical settings. Neutrophils and macrophages rapidly infiltrate the kidney after renal ischemia-reperfusion injury. Chemokines are a large family of secreted proteins that together coordinate leukocyte trafficking and activation during homeostasis, development and inflammation. In many animal models of inflammatory kidney disease, various chemokines and chemokine receptors contribute to tissue injury.
The CC chemokine receptor-1 ( CCR1) is a prime therapeutic target for treating autoimmune diseases. Since CCR1 is known to mediate the migration of lymphocytes and macrophages into inflamed tissue, CCR1 appeared to be a promising target for a blocking strategy. CCR1 also plays an important role in mediating the infiltration of mononuclear cells and subsequent renal fibrosis after unilateral ureter obstruction. Therefore, researchers have developed potent CCR1 antagonists.
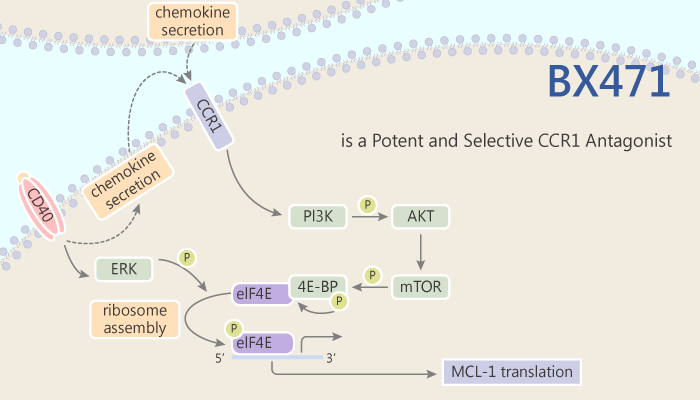
The lead compound BX471 is currently in phase I human trials. Especially, BX471 is a functional antagonist for mouse CCR1. BX471 effectively ameliorates disease in a rat experimental allergic encephalomyelitis model. BX471 delays the rejection of rat heart and rabbit renal transplants. Moreover, BX471 reduces the infiltration of macrophages, lymphocytes, and, more specifically, CCR5-positive CD8 T cells infiltrating the obstructed kidney. Pretreatment of WT mice with BX471 also suppresses neutrophil and macrophage infiltration in the model. Moreover, administration of BX471 markedly reduces macrophage and T cell infiltrates, and reduces tubular injury and interstitial fibrosis in diverse mouse models of kidney disease.
In summary, BX471 is a potent functional antagonist based on its ability to inhibit a number of CCR1-mediated effects including Ca2+ mobilization, increase in extracellular acidification rate, CD11b expression, and leukocyte migration.